Estimated reading time: 8 minutes
Table of contents
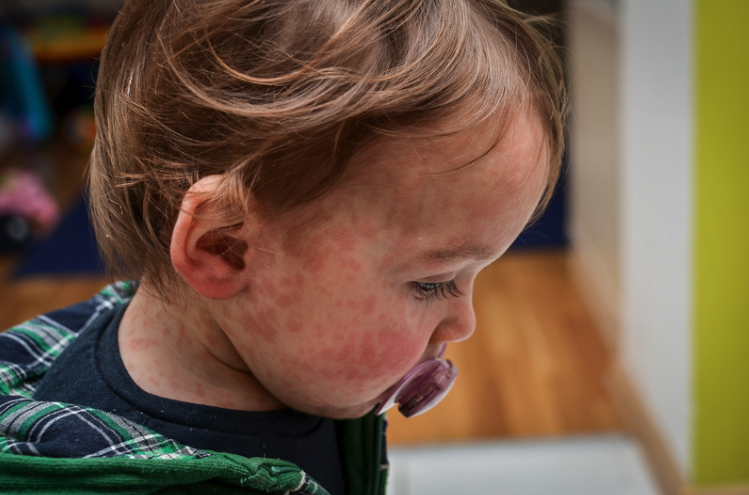
As we begin to officially enter the Winter season, may start to feel those telltale signs of respiratory illness – a tickle in your throat, more sniffles than usual, a sharp headache. Could it be the flu? With elevated flu activity across the nation and positive cases growing in our region this month, it just might. Let’s break down everything you need to know about the flu – from symptoms and treatments, to preventative measures.
Symptoms of the Flu
Flu is the short name for Influenza, a virus that affects your respiratory system including your nose, throat, and lungs. There are 4 types of influenza – A, B, C, and D. Flu A and Flu B are what we most commonly see during our “flu season” which is typically during the Fall and Winter, with activity often peaking during the month of February.
Symptoms of flu may look similar to other illnesses, including:
- Fever
- Chills
- Headache
- Cough
- Fatigue
- Body aches
- Sore throat
- Stuffy nose
Sound familiar? A key difference in deciding if it’s a common cold or the flu is the speed of symptom onset. The common cold may start to give you hints of its arrival in the days before you feel full-blown sick, whereas the flu often gives people very sudden, severe symptoms. A popular description we also hear from patients in clinical practice is when it’s the flu, you feel like you’ve been “hit by a truck”. People infected with influenza are also at greater risk of developing secondary infections, such as ear infections or pneumonia. Consult with your healthcare provider if you are concerned about your symptoms.
How To Know If You Have the Flu
The flu is a virus and can be difficult to distinguish between other seasonal colds we get throughout the year. This is why testing is important for data, although during peak times, healthcare providers in busy environments may diagnose flu based on clinical examination and regional data vs. using a test, because laboratories may be overwhelmed and tests that are sent out may not come back in a timely manner. You may hear the term “influenza-like illness” or “ILI” which is a term used to diagnose the likelihood of flu if a specific diagnostic test wasn’t conducted. However, at Concierge Pediatrics, we will simply conduct a flu test.
A flu test is administered by swabbing deep inside the inside of the nose, called a nasopharyngeal swab. A rapid influenza diagnostic test (RIDT) is an antigen test that will determine flu presence within about 15-20 minutes. The benefit of an RIDT is that you can get results quickly while in the office or at home, but they are not as sensitive as other tests so you can test negative and still have the flu. This type of test is now more common to find over-the-counter at your local pharmacy, unlike in the past. Other tests, like reverse transcription polymerase chain reaction (RT-PCR) tests are done with a similar collection method, and then sent out to a lab for extended testing. This can sometimes only take a few hours, but depending on the time it takes to be picked up and brought to a laboratory, plus volume of total tests received by the lab, it can take up to a few days.
At Concierge Pediatrics, we run a 15-minute PCR test to guarantee quick results. We can also provide an optional respiratory viral panel test to understand what other virus your illness may be, if not influenza.
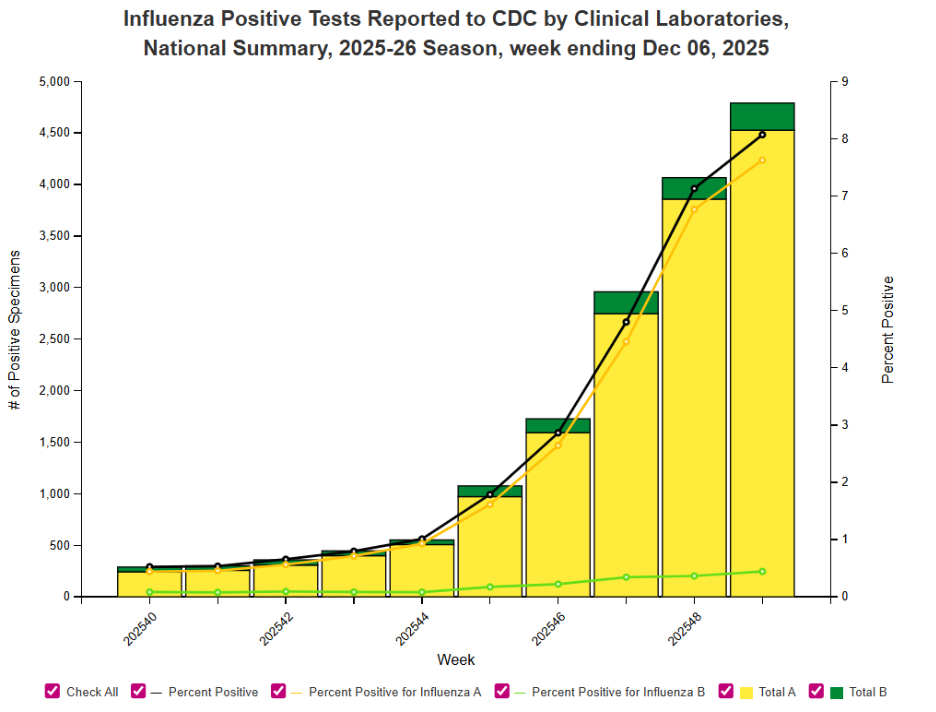
Current flu data in our region from CDC.gov
Flu Treatment and Medications
For the most part, treatment of the flu is the same as it is for the common cold. It is important to focus on the hallmarks of good self care, including quality sleep, nourishment, hydration, and rest, as well as supportive care methods to treat symptoms. Supportive care methods include a mix of medicine and proven home remedies, such as:
- ibuprofen (Motrin, Advil, etc.) and acetaminophen (Tylenol etc.) for pain and discomfort from fever or body aches
- honey for a cough in ages 2+ years*
- cool mist humidifiers to help loosen mucous
- sterile saline rinses to clear nasal passages
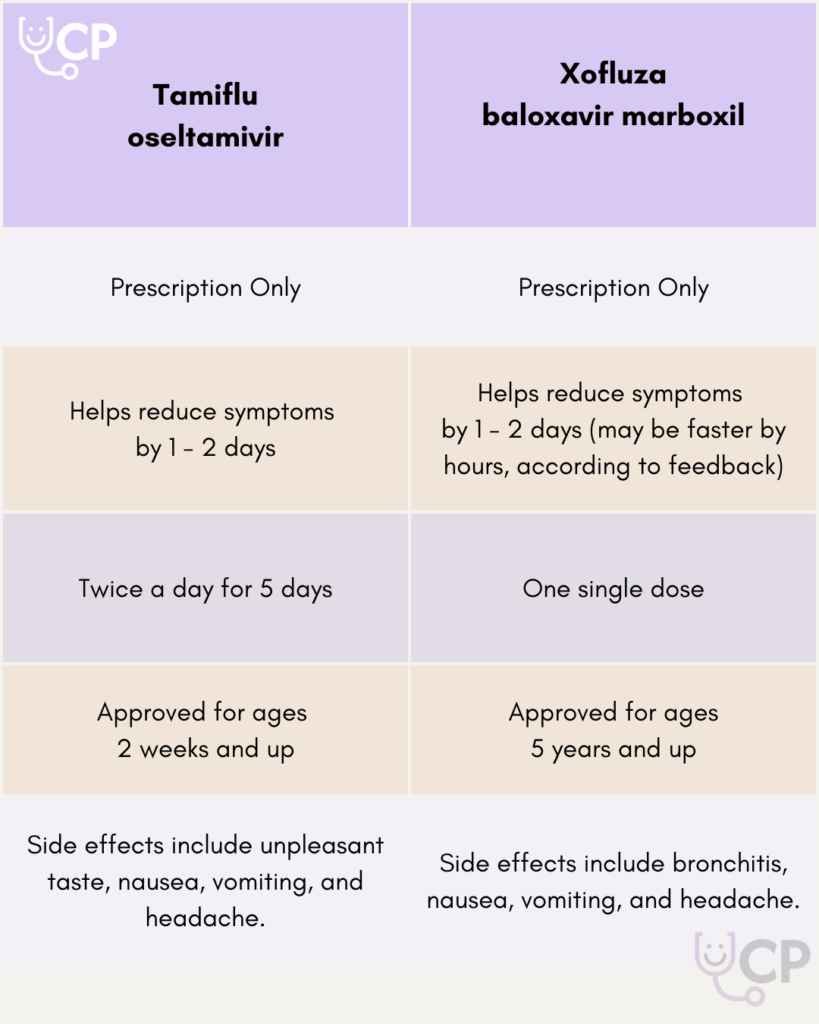
The flu is a virus, so antibiotics will not help you recover, as those are targeted to treat bacteria. However, some people may want to opt for a prescription anti-viral treatment, like oseltamivir (i.e.; Tamiflu) or baloxavir marboxil (i.e.; Xofluza). These medications are most effective when taken within 48 hours of symptom onset. Some of the drawbacks of these medications include reported unpleasant side effects, like a strong, bitter taste, nausea, vomiting, and sometimes confusion or bronchitis. For this reason, the drugs are usually recommended for immunocompromised individuals, and those under age 5 or over age 65. The benefit is that these drugs may reduce the duration of your symptoms when taken right away. Discuss the pros and cons with your healthcare provider so you can make the decision that’s best for your family!
How Can I Avoid the Flu?
The flu is an airborne illness, meaning it can spread via droplets from an infected person when they speak, cough, or sneeze. It is also possible to become infected when the droplets of an infected person touch a surface, and the next person touches the surface followed by their nose, mouth, or face.
An infected person can unknowingly spread the virus the day before they start to feel symptoms, and up to a week after becoming sick, but they are most contagious during their first 3 days of symptoms. For the sake of public health, this is why it is very important to stay home if you’re not feeling well, as much as possible, and to mask if you must leave the house when not feeling well. If a person infected with the flu is able to isolate in 1 room or area the house and use a dedicated bathroom, this will help to prevent the spread to other household members. If they’re unable to do so, they can simply follow fundamental public health measures, such as
- covering their cough and sneeze into their elbow
- good handwashing practices
- proper disposal of used tissues
- get a flu shot
Other household members should also remember to practice self care measures and frequently wash their hands with soap and water for at least 20 seconds. People with the flu can begin to return to their normal activities once they are feeling better and have been fever-free for 24 consecutive hours.
Clean high-touch surfaces, like doorknobs, light switches, countertops, bathrooms, toys, tv/gaming controls, and phones. Soap and water is usually fine, or you can use a diluted solution of household bleach and water.
Is it Too Late to Get a Flu Shot?
In the 2023-2024 season, a record 200+ pediatric deaths tragically occurred from influenza infection. The very best way to prevent the flu from hitting your household is to get an annual flu vaccine. It’s not too late to get a flu shot! Flu shots are offered at Concierge Pediatrics as part of your membership well care, and usually also for free at local pharmacies.
The flu vaccine has been researched, studied, and tested extensively for 80+ years and we do recommend getting it for ages 6 months and above. We also have the FluMist nasal spray available, so kids don’t have to feel fearful about a needle. The nasal spray is not recommended for people who are immunocompromised, nor those with asthma.
Scientists work hard to determine what the dominant flu strain is likely to be and then try to match that each year’s vaccine to the strain of flu we expect to see for the upcoming flu season. Because the flu is a virus, it means that it can evolve and still infect someone who has already gotten the vaccine. While we recognize this can be a disappointment when you feel like you’ve done the work to prevent falling ill, the important thing we will note is that the symptom severity and illness duration of a vaccinated vs. unvaccinated child with the flu are very different. If you are unsure about vaccination, talk to a trusted healthcare provider, such as any physician at Concierge Pediatrics. We will talk through your concerns and provide you with evidence-based resources to arm you with information so you can confidently make an informed decision.
The flu vaccine takes about 2 weeks to take full protection effect, and it is recommended to get the flu shot each year before Halloween (flu before Boo!), but people can be vaccinated through the month of April to be protected.
At Concierge Pediatrics, we’re here to take care of your family in health, spirit, and education. If you have flu questions, let us know! We’re here to get through flu season together.
*honey and products containing honey should NOT be given to babies under 1 year old. Honey may contain botulism spores, which are harmful to babies under 1 year old. Botulism spores are harmless for babies over 1 year old, as their immune systems and digestive tracts become more mature at that age.